Feeding via a tube
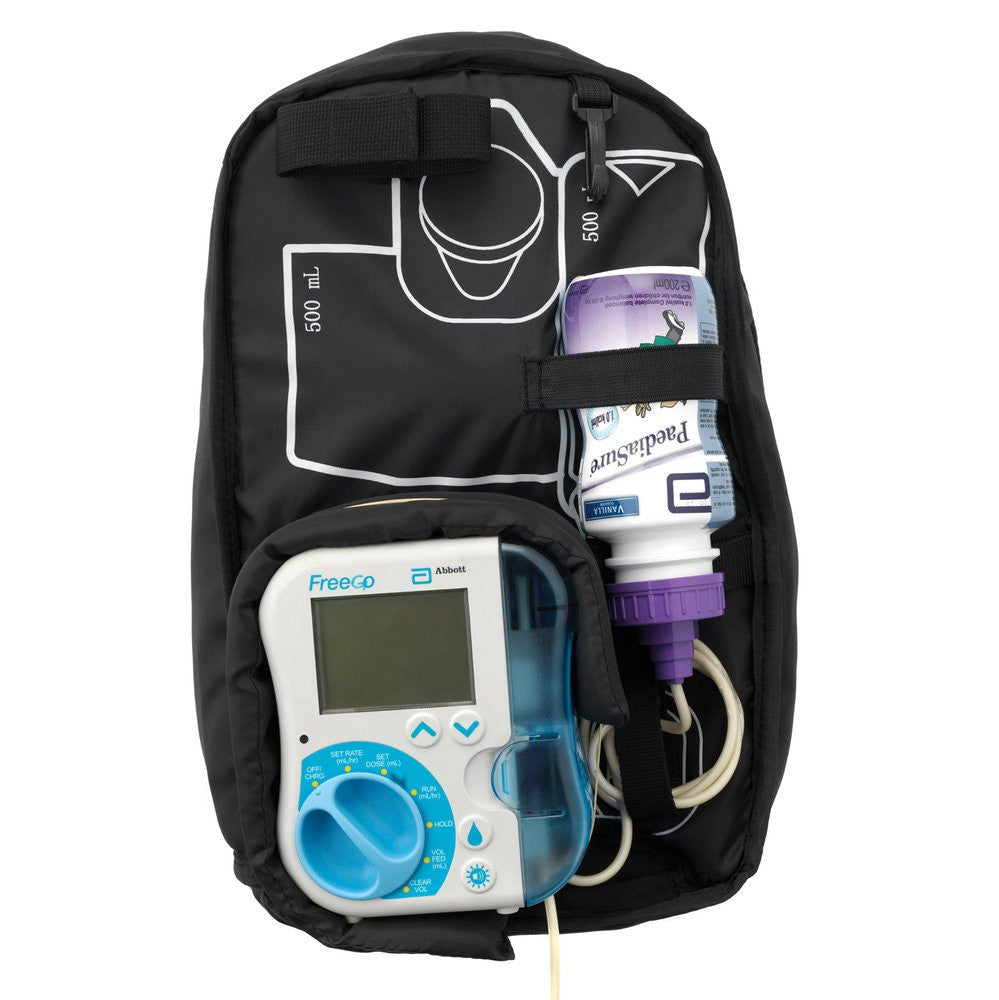
Feeding via a tube – why would my child be fed through a pump?
Feeding via a tube is often a consequence of a brain injury. Swallowing is a very complex process, and poses several risks. In cases like this, your child will need feeding via a tube. This is so they can receive enough nutrition. The tube will also be used to keep your child hydrated, and may also be used for some medications. This is the case for our child LB, who is fed via a nasogastric (NG) tube.
What is a nasogastric (NG) tube for feeding?
An NG tube is a thin, soft plastic tube. It is inserted through your child’s nose, and into the stomach. This allows a child to be fed, hydrated and medicated. Having feeds this way is known as ‘enteral feeding’. There are a number of alternatives to NG tubes, and we will look at them in a separate post.
How long will my child have an NG tube?
Some children only need an NG tube for a few days while in hospital. Other children need an NG tube because they have difficulty chewing or swallowing.
Brain injuries can cause people to become breathless and tire easily when eating. The timeline will depend on what your child’s specific feeding difficulties are. These will be reviewed by a gastroenterology team.
What are the advantages and disadvantages of feeding via an NG tube?
Advantages include providing a safe method of feeding or administering medication. The tube can also be inserted or removed without medication or surgery. Parents or carers can be trained in inserting the tube, otherwise its done by a professional.
Disadvantages are:
- the tube is visible on your child’s face, which can be challenging to adapt to.
- insertion of the tube can upset a child as it can be uncomfortable.
- if incorrectly inserted, it could go into the lungs and heighten the risk of aspiration.
- there is a risk of tissue damage as the tube can rub against the skin.
Inserting an NG tube
An NG tube will generally be inserted by a registered nurse. The initial insertion will be while your child is an inpatient in hospital. The length and size of tube depends on your child’s size, which will be measured.
The nurse will insert one end of the tube into your child’s nostril. If they previously had a tube, the other nostril will be used. This is done to reduce irritation on the skin and potential tissue damage.
Once the tube has been inserted, it will be tested to ensure it is correctly sited. It will then be secured to your child’s cheek with adhesive tape. A soft dressing such as DuoDerm, is placed on your child’s cheek for protection. Your child needs to be awake during the insertion of the tube.
How long does an NG tube last for?
This comes down to the specific NG tube that is used. Some last up to 90 days, and others only last 30 days.
Checking the location of the tube
One risk is the tube is in the lungs instead of the stomach. The tube can move if it is accidentally pulled or if your child has vomited. This can cause feed or medication to go into your child’s lungs. If this happens, it can cause infection or a potentially life-threatening situation.
To prevent this, an NG tube should be checked every time before usage. In hospital, this may be done by x-ray. Outside hospital, the tube is checked by using a pH strip to measure acidity. If it is in the stomach, the test strip will indicate acidity. To check, simply use a syringe and then drip it onto the pH strip. Different strips have different colours, which are generally displayed on a container. You are looking for a pH of 6 or less.
Some medications affect the result of the pH test. An example of this is anti-reflux medication such as Omeprazole or Lansoprazole. Your clinician should advise you if this is the case.
What if the pH reading is too high?
Do not put anything down the tube if unsure of the tube position. If you don’t get the right pH reading, you should try again after 10 minutes. This is the same if you cannot get any fluid. You can also switch to a bigger syringe.
If this doesn’t work, try turning your child onto their left hand side. The tube should then reach the stomach contents needed for the positioning to be verified. If after an extended period you are still unable to get a reading, seek medical advice.
How to use the NG tube to administer feeds, water or medicines
Small amounts of medicines or water can be slowly pushed into the NG tube using a syringe. You should be shown how to do this by a nurse or suitably qualified medical practitioner. When giving your child feeds or formula, this will generally be via a pump over a period of time. A dietician will determine the appropriate way to ensure your child can get enough nutrition.
When using a pump, you firstly need to know the speed of the feed and the size of the dose. There are a number of different feeds that may be used. Once the feed is ready, if will need to be primed through a giving set. This prepares the pump for connection to the tube.
Your child should be placed at an angle of at least 30 degrees. If they are flat, there is a risk they could choke or become distressed. After testing, the tube should be flushed with sterile water to ensure it is clear before feeding commences.
How to use a feeding pump
A medical practitioner will show you how to use your child’s specific pump. The pump will alert you when the feed cycle is complete. You should then flush the tube to ensure it is clear of feed. You should ensure you are observing your child the entire time they are using a pump. This is because there is a risk of choking, or for an occlusion to occur if the tube becomes kinked in any way. If their breathing significantly increases or they change colour you may want to pause the feed to ensure they are okay.
Medicines via an NG tube
If your child is receiving medications through an NG tube, it is important that they are safe to go down the tube. Most medicines are available in liquid form that can be easily pushed down the tube. Some tablets can be crushed and dissolved in water to then be passed down the NG tube. It is important you check that tablets can be given enterally. Some medicines are not safe to be crushed.
Never mix medicines together before putting into the NG tube, as there may be adverse interactions. Flush the NG tube with water before, between and at the end of giving medicine.
Getting additional supplies
You should be advised how to order any replacement NG tubes, syringes and other equipment you may need at home. Arrangements for this vary in local areas. For LB, this is done via our dietician on a monthly basis. Community based teams do not always have access to NG tubes or tapes, so you should ensure you have spares available at home for emergency situations.
How to care for your child and their tube
Even if your child is not eating, you must continue to clean their mouth regularly and brush their teeth. To protect their skin, use a protective adhesive pad such as DuoDerm to prevent rubbing and tissue damage. Tube tapes should be changed regularly if they are starting to come loose or become dirty.
Bathing, showering and swimming
Your child will be able to bath or shower safely if the cap on the end of the NG tube is securely closed. When swimming, ensure that the tape securing the tube to your child’s cheek is waterproof. Replace the tape as soon as it becomes damp to lessen the risk of the tube becoming dislodged.
Going to school
Your child will be able to go to school as normal.
Holidays
When going on holiday or travelling, it is important to be organised ahead of time. You must ensure you have sufficient supplies for your trip. If going abroad, get a doctors letter stating that you are carrying medical supplies. This may help with airport security.
If your child has a cold
You need to pay particular attention to keeping your child’s nose clear of secretions. This is important, because the tube makes one of their nostrils smaller than the other. This may mean that they work harder to breathe, which can lead to complications.
Sources of Further Information
https://www.nestlehealthscience.co.uk/mychildwithcerebralpalsy/nutrition/tube-feeding-basics
https://infokid.org.uk/supporting-information/feeding-your-baby-or-child-with-chronic-kidney-disease/using-feeding-devices/